- Visibility 86 Views
- Downloads 13 Downloads
- DOI 10.18231/j.ijca.2022.066
-
CrossMark
- Citation
Comparison of videolaryngoscopy and direct laryngoscopy for tracheal intubation in paediatric patients
- Author Details:
-
Nipun Yallawar
-
Janhavi Thatte
-
Shripad Mahadik
-
Deepak Phalgune *
Introduction
Many attempts are made to improve the techniques and tools of direct laryngoscopes since its inception. A “line of-sight” from the operator and the laryngeal inlet is the basis of the direct laryngoscopy (DL). The position of the head and dependable anatomy is very important for the success of DL. If there is poor tissue mobility, limited mouth opening, or enlarged tongue, the chances of intubation by DL decrease.[1], [2] The accomplishment of tracheal intubation increases if video laryngoscopy (VL) is used. The success rate of VL is more because high-resolution micro-cameras and small portable flat-screen monitors are used in video laryngoscope. It is reported that VL is useful in everyday and complex tracheal intubation, especially in children.[3]
The airway anatomy of the children is distinctive as compared with adults. The laryngoscopy and intubation in children is difficult because of restricted opening of the mouth, comparatively larger tongue and more cephalad larynx; so also the consumption of oxygen is much higher in children as compared to the adults. Hence, limited period is available for the intubation in the children.[4] The presence of congenital orofacial clefts distort the upper airway anatomy and association with wider palatal clefts, bilateral cleft lips, major nasal deformity, micrognathia and receding mandible further increases the intubation difficulty.[5]
In VL, a flexible endoscope is used for indirect laryngoscopy and in VL, there is no need of a direct line to view the airway structures. The glottis can be visualized more correctly by VL. A small quantity of force is required at the base of the tongue during VL. Hence, the chances of local tissue injury and response to stress are reduced. Even though there is no obvious evidence that the success of endotracheal intubation (ETI) is increased by VL, VL is now widely used by the anaesthesiologist and other healthcare providers. A further research should be conducted to ascertain whether VL improves intubation time, ETI and first-attempt success rates and thus can become a probable substitution to conventional DL. Even though there is an improved visualization of the glottis by using VL, difficulty may arise in ETI. An anaesthesiologist may develop a false sense of security and may not be prepared for ETI of difficult airway.[6] Procedure is more complicated and expensive. It was reported that there is a benefit of using VL.[7], [8] There are many studies in adults but data on paediatric population in India is lacking. The present study was aimed to compare the efficacy of VL and DL for ETI in children.
Materials and Methods
This randomised controlled study was conducted between May 2020 and February 2021 in the major operation theatre of a tertiary care hospital, Pune, India. After approval from the institutional ethics committee, written informed consent was obtained from all the parents /guardians prior to enrollment explaining the risks and benefits of the procedure. Children aged between one and five years posted for elective surgery under general anaesthesia, falling into American Society of Anaesthesiologist (ASA) grades I-II and Cormack-Lehane grade I and II were included. The exclusion criterion was refusal of parents /guardians to participate in the study.
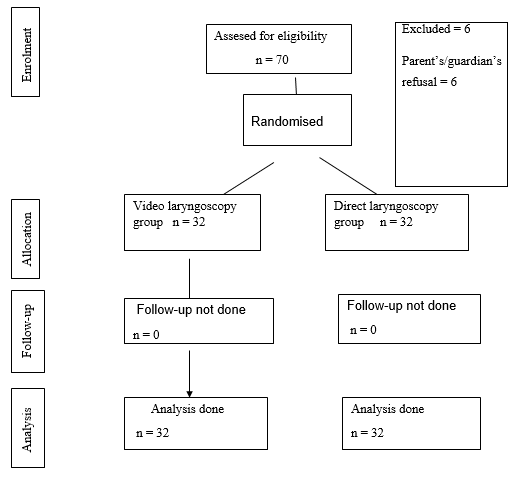
Out of 70 patients assessed for eligibility, after exclusion, 64 children were randomly divided into two equal groups of 32 each with the help of www.randomizer.org ([Figure 1]). The program was known as research randomizer. The program produced two sets of random numbers out of the range of numbers provided (for e.g. 1- 64) by taking user input on having uniqueness of the numbers to be generated. For the present study, the program produced two sets of 32 unique numbers per set. The sheet of the random numbers was ready before the study was started. The children were randomly divided into two groups; Group I – VL and Group II – DL.
All the children were thoroughly examined before the procedure. Basic investigations such as complete blood count, chest X-ray, etc. were done to rule out major systemic illness. An airway assessment of the children was done on size and shape of head, facial features, mandibular size and symmetry, tongue size, palatal shape and pathology, prominence of teeth especially upper incisors, range of motion of head and neck. Airway assessment was done by Copur score[9] and Cormack Lehane grading system.[10]
In the operating room, standard basic monitoring devices were attached to the children including a pulse-oximeter, 3 lead ECG, and non-invasive blood pressure (NIBP). Baseline measurements of NIBP, heart rate and saturation were recorded. Intravenous (IV) access was obtained. Appropriate size endotracheal tube for the children was selected. The tube was lubricated with a water soluble jelly. Children were pre-oxygenated with 100.0% oxygen for 5 min. Induction was done with Inj. thiopentone 5mg/kg + Inj. atracurium 0.5 mg/kg. Children were ventilated with bag and mask with sevoflurane 2.0% and oxygen for 3 min. After optimal positioning, stop watch was started as video laryngoscope inserted in the mouth. Time was noted when best possible view of glottis was seen. The endotracheal tube was passed through the vocal cords and successful insertion time was recorded. The VL was done with the blade being introduced in the midline without tongue lateralisation. Glottis was visualized on monitor.
If the intubation attempt with VL failed but saturation was maintained, another attempt was made for intubation and if the saturation decreased mask ventilation with 100.0% oxygen followed by intubation with video laryngoscope was carried out. Similar steps were taken for DL. Maximum 3 attempts were tried in each type of laryngoscopy. However, even after 3rd attempt the child could not be intubated, the other type of laryngoscopy was tried and these children were excluded from the study.
Time to the best visualization (TTBV) of glottis was defined as the time from when the laryngoscope blade entered the patient’s mouth to the time the anaesthesiologist determined that the best possible view of glottis (Cormack-Lehane grade I or II) had been achieved.[11] The time to intubate (TTI) was defined as the time required between the insertion of the laryngoscope into the oral cavity and the view of the tube crossing the glottis or, in blind tracheal intubation, the presence of a carbon dioxide wave in the exhaled breath.[12] An attempt was defined as the insertion of the endotracheal tube into the trachea via the glottis under visualisation using a laryngoscope within 60 s. Inability to pass the endotracheal into the glottis within 60 s was considered a failure of the first attempt.[13]
The primary outcome measure was to compare the time required for best visualisation of glottis, whereas secondary outcome measures were to compare TTI and number of attempts. Donoghue AJ et al. reported that the first-attempt success in 81.0% and 39.0% of subjects in VL and DL respectively.[3] The sample size of 30 patients in each group was calculated by formula N[14] = {2pav (1-pav) (Zα + Zβ)2} /Δ2. Zα (a standard normal variate at 1% type 1 error) was taken as 2.58, whereas Zβ (a standard normal deviate for β power at 80% type II error) was taken as 0.842. We included 32 children to validate the results.
Statistical analysis
Data were collected and was analysed by using Statistical Package for Social Sciences for Windows, Version 20.0 from IBM Corporation Armonk, NY, USA. The data on categorical and continuous variables are presented as n (% of cases) and mean ± standard deviation (SD) respectively. The Chi-square/Fisher’s exact test and unpaired student’s t-test were used to compare the qualitative and quantitative variables respectively. A p-value < 0.05 was considered as a significant.
Results
Out of 70 children, 64 children were included in the study as shown in [Figure 1]. They were divided into two groups (VL and DL) by randomization. As depicted in [Table 1], the two groups were comparable in terms of the mean age, gender and ASA grades. The mean Copur score was 6.1 ± 1.5 and 6.4 ± 2.2 in VL and DL groups respectively (p-value = 0.430) As shown in [Table 2], the percentage of children in Cormack-Lehane grade I and grade II in VL group were 29/32 (90.6%) and 3/32 (9.4%) respectively, whereas the percentage of children in Cormack-Lehane grade I and grade II in DL group were 22/32 (68.7%) and 10/32 (31.3%) respectively (p-value = 0.007). It can be seen from [Table 3] that mean TTBV (in seconds) was 6.1 ± 1.2 and 5.3 ± 1.1 in VL and DL groups respectively (p-value = 0.010), whereas mean TTI (in seconds) was 15.3 ± 1.9 and 13.1 ± 2.2 in VL and DL groups respectively (p-value = 0.001). The number of items required for intubation were comparable between VL and DL groups (p-value = 0.580).
|
Characteristics |
VL n = 32 (%) |
DL n = 32 (%) |
Total n = 64 (%) |
p- value |
|
Mean age (in years) ± SD |
3.0 ± 1.3 |
2.6 ± 1.4 |
|
0.170* |
|
Gender |
|
|
|
|
|
Males |
18 (56.3) |
23 (71.9) |
41(66.1) |
0.460** |
|
Females |
14 (44.7) |
9 (28.1) |
21(33.9) |
|
|
ASA Grades |
|
|
|
|
|
Grade I |
29 (90.6) |
27 (84.4) |
56 (87.5%) |
0.807*** |
|
Grade II |
3 (9.4) |
5 (15.6) |
8 (12.5%) |
|
Characteristics |
VL n = 32 (%) |
DL n = 32 (%) |
Total n = 64 (%) |
p- value |
|
Mean Copur score ± SD |
6.1 ± 1.5 |
6.4 ± 2.2 |
|
0.430* |
|
Copur score |
|
|
|
|
|
Easy intubation (5-7) |
28 (87.5%) |
29 (90.6%) |
57 (89.1) |
0.460** |
|
Moderately difficult (8-10) |
3 (9.4%) |
2 (6.3%) |
5 (7.8) |
|
|
Difficult airway (> 10) |
1 (3.1%) |
1 (3.1%) |
2 (3.1) |
|
|
Cormack-Lehane grades |
|
|
|
|
|
Grade I |
29 (90.6%) |
22 (68.7%) |
51 (82.3%) |
0.007** |
|
Grade II |
3 (9.4%) |
10 (31.3%) |
11 (17.7) |
|
|
Characteristics |
VL n = 32 (%) |
DL n = 32 (%) |
Total n = 64 (%) |
p- value |
|
TTBV in sec ± SD |
6.1 ± 1.2 |
5.3 ± 1.1 |
|
0.010* |
|
TTI in sec ± SD |
15.3 ± 1.9 |
13.1 ± 2.2 |
|
0.001* |
|
Number of attempts |
|
|
|
0.580** |
|
One |
29 (90.6%) |
28 (87.5%) |
57 (89.1) |
|
|
Two |
3 (9.4%) |
4 (12.5%) |
7 (10.1) |
Discussion
The airway and respiratory complications during the perioperative period in paediatric anaesthesia are common leading to morbidity and mortality.[15] These complications can be seen in healthy children, particularly infants. It is reported that the incidence of difficult laryngoscopy is more common in infants and neonates.[16] The airway of the children is distinctly different from that of adults, hence the knowledge of the airway anatomy and physiology of children is very important to prepare for managing children’s airway.[17], [18] Due to these anatomical and physiological differences, the anaesthesiologist may come across unexpected difficulty in laryngoscopy and intubation in children while using conventional DL with Macintosh blade. Indirect VL in children is possible because of recent inventions in optics and electronics devices. There is no need to align the line of sight with laryngeal inlet in indirect VL hence it is advantageous for intubation in children as compared to DL.[19] Many studies have compared VL with DL for tracheal intubation and opined that VL is better than DL.[4], [20], [21], [22], [23]
In the present study, the mean TTBV of VL and DL was 6.1 sec and 5.3 sec respectively (p-value = 0.010). Our findings are consistent with previous studies.[4], [24] Fiadjoe JE et al reported that the median TTBV was 9.9 sec and 8.1 sec in DL and VL groups respectively (p-value = 0.03).[21] Vlatten A et al. reported that the median TTBV in DL and VL was 5.5 sec and 7.0 sec respectively (p-value = 0.769).[25] Sun Y et al. reported that the time of intubation was increased but glottis was better visualized by VL.[4] Javaherforooshzadeh F and Gharacheh L reported that the glottis was better visualized by VL than DL.[26] Macnair D et al. opined that glottis was better visualized by VL, but TTI was higher as compared to DL.[24] Karsli C et al. concluded that in children with a difficult airway, laryngoscopic view was better in VL than DL. The study further stated that DL and VL required 20 sec and 26 sec respectively to achieve the adequate view of the glottis (p-value = 0.5).[27]
In the present study, of 32 children on whom VL was performed, 29 (90.6%) were intubated in first attempt while 3 (9.4%) required second attempt for intubation, whereas in DL group, of 32 children, 28 (87.5%) were intubated in first attempt and 4 (12.5%) required second attempt (p-value = 0.580). Fiadjoe JE et al. reported that the success rate of VL and DL was 96.0% and 94.0% respectively (p-value > 0.05).[21] Javaherforooshzadeh F and Gharacheh L reported that 22, 8 and 6 patients were intubated in 1st, 2nd and 3rd attempt respectively in DL group, whereas 24, 6 and 2 patients were intubated in 1st, 2nd and 3rd attempt respectively in VL group (p-value = 0.033).[26]
Abid ES et al. reported that first pass success (FPS) in children above one year of age was better as compared to DL.[28] Similar results were reported by Eisenberg et al. in a paediatric emergency medicine department.[29] Rabiner JE et al. reported that in DL group, 15 (60.0%) and 5 (20.0%) were intubated in the first and second item respectively, whereas in VL group, 16 (64.0%) and 4 (16.0%) were intubated in the first and second item respectively which was not statistically significant.[30]
The intubation procedure can be recorded by VL. The same can be reviewed for teaching purposes to calculate the number of attempts and time to intubation and adverse events.[31] The objective assessment of procedural performance can be done by VL and it is more precise than self-report.[32]
In our study, the mean TTI of VL was 15.3 sec while that of DL was 13.1 sec (p-value = 0.001). Fiadjoe JE et al. reported that the median TTI was 22.6 sec and 21.4 sec in the VL and DL group respectively (p-value= 0.24).[21] Macnair D et al. reported that the median TTI was 16.0 sec and 22.5 sec for DL and VL respectively (p-value < 0.001).[24] Vlatten A et al. reported that the median TTI in DL and VL was 21 sec and 27 sec respectively (p-value = 0.006).[25] Javaherforooshzadeh F and Gharacheh L reported that TTI was 29.33 sec and 33.33 sec for DL and VL groups respectively (p-value = 0.20).[26] Rabiner JE et al. reported that the mean TTI was 67.4 sec and 61.4 sec in DL and VL group respectively (p-value > 0.05).[30]
White M et al reported in a study conducted among anaesthesiologists and paediatric intensivists that there was no significant difference in TTI between VL and DL. The study further stated that in general satisfaction was higher in DL as compared to VL and in case of emergency intubation the higher percentage would choose DL over VL.[33] Lim T et al. reported that 85.0% and 30.0% of anaesthesiologists preferred DL in an easy and difficult airway scenario respectively, even though time to intubation was significantly shorter in VL as compared to DL.[34] Platts‐Mills TF reported that in an emergency department DL was preferred over VL.[35] It was observed that in difficult airway situation where it is hard to introduce the endotracheal tube between the vocal cords with the VL technique, TTI is longer in new learners.
The strength of the present research is that it was probably the first study conducted in children between one and five years in Indian population. Limitations to the current analysis warrant consideration. The present research was conducted in only one institution with small population size which included ASA grade I and II and Cormac and Lehane score 1 and 2. The grades of Cormack and Lehane classification of laryngeal views are subjective. The blinding was not done in the present research. Complications were not noted and compared. These findings should be considered hypothesis generating and need to be confirmed in larger populations by conducting randomized controlled studies.
Conclusions
From the above study, it can be concluded that the efficacy of direct laryngoscopy is better than videolaryngoscopy for best visualization of the glottis and endotracheal intubation in paediatric patients.
Source of Funding
None.
Conflict of Interest
None.
References
- B Finucane, BCH Tsui, A Santora. . Principles of airway management 2011. [Google Scholar]
- F Agro, G Barzoi, F Montecchia. Tracheal intubation using a Macintosh laryngoscope or a GlideScope in 15 patients with cervical spine immobilization. Br J Anaesth 2003. [Google Scholar]
- AJ Donoghue, AM Ades, A Nishisaki, ES Deutsch. Videolaryngoscopy versus direct laryngoscopy in simulated pediatric intubation. Ann Emerg Med 2013. [Google Scholar]
- Y Sun, Y Lu, Y Huang, H Jiang. Pediatric video laryngoscope versus direct laryngoscope: a meta-analysis of randomized controlled trials. Paediatr Anaesth 2014. [Google Scholar]
- A Sharma, P Durga, I Gurajala, G Ramchandran. An observational study of the feasibility of Airtraq guided intubations with Ring Adair Elvin tubes in pediatric population with cleft lip and palate. Anesth Essays Res 2015. [Google Scholar]
- JB Paolini, F Donati, P Drolet. Video-laryngoscopy: another tool for difficult intubation or a new paradigm in airway management?. Can J Anaesth 2013. [Google Scholar]
- S Thong, Y Lim. Video and optic laryngoscopy assisted tracheal intubation-the new era. Anaesth Intensive Care 2009. [Google Scholar]
- LM Pott, WB Murray. Review of video laryngoscopy and rigid fiberoptic laryngoscopy. Curr Opin Anaesthesiol 2008. [Google Scholar]
- G Lane. Intubation techniques. Oper Tech Otolaryngol Head Neck Surg 2005. [Google Scholar]
- R Krage, CV Rijn, DV Groeningen, SA Loer, LA Schwarte, P Schober. Cormack-Lehane classification revisited. Br J Anaesth 2010. [Google Scholar]
- RS Cormack, J Lehane. Difficult tracheal intubation in obstetrics. Anaesthesia 1984. [Google Scholar]
- JC Koh, JS Lee, YW Lee, CH Chang. Comparison of the laryngeal view during intubation using Airtraq and Macintosh laryngoscopes in patients with cervical spine immobilization and mouth opening limitation. Korean J Anesthesiol 2010. [Google Scholar]
- M Manirajan, PU Bidkar, RK Sivakumar, S Lata, G Srinivasan, AK Jha. Comparison of paediatric King Vision TM videolaryngoscope and Macintosh laryngoscope for elective tracheal intubation in children of age less than 1 year: A randomised clinical trial. Indian J Anaesth 2020. [Google Scholar]
- H Motulsky. . Intuitive Biostatistics 1995. [Google Scholar]
- N Jimenez, KL Posner, FW Cheney, RA Caplan, LA Lee, KB Domino. An update on pediatric anesthesia liability: a closed claims analysis. Anesth Analg 2007. [Google Scholar]
- S Heinrich, T Birkholz, H Ihmsen, A Irouschek, A Ackermann, J Schmidt. Incidence and predictors of difficult laryngoscopy in 11.219 pediatric anesthesia procedures. Paediatr Anaesth 2012. [Google Scholar]
- L Adewale. Anatomy and assessment of the pediatric airway. Paediatr Anaesth 2009. [Google Scholar]
- J Harless, R Ramaiah, SM Bhananker. Pediatric airway management. Int J Crit Illn Inj Sci 2014. [Google Scholar]
- K Lingappan, JL Arnold, CJ Fernandes, M Pammi. Videolaryngoscopy versus direct laryngoscopy for tracheal intubation in neonates. Cochrane Database Syst Rev 2018. [Google Scholar]
- JT Kim, HS Na, JY Bae, DW Kim, HS Kim, CS Kim. GlideScope video laryngoscope: a randomized clinical trial in 203 paediatric patients. Br J Anaesth 2008. [Google Scholar]
- JE Fiadjoe, H Gurnaney, N Dalesio, E Sussman, H Zhao, X Zhang. A prospective randomized equivalence trial of the GlideScope Cobalt® video laryngoscope to traditional direct laryngoscopy in neonates and infants. Anesthesiology 2012. [Google Scholar]
- H Mutlak, U Rolle, W Rosskopf, R Schalk, K Zacharowski, D Meininger. Comparison of the Tru View infant EVO2 PCD TM and C-MAC video laryngoscopes with direct Macintosh laryngoscopy for routine tracheal intubation in infants with normal airways. Clinics 2014. [Google Scholar]
- MC White, CJ Marsh, RM Beringer, JA Nolan, AY Choi, KE Medlock. A randomised, controlled trial comparing the Airtraq™ optical laryngoscope with conventional laryngoscopy in infants and children. Anaesthesia 2012. [Google Scholar]
- D Macnair, D Baraclough, G Wilson, M Bloch, T Engelhardt. Pediatric airway management:comparing the Berci-Kaplan Video Laryngoscope with direct laryngoscopy. Paediatr Anaesth 2009. [Google Scholar]
- A Vlatten, S Aucoin, S Litz, B Macmanus, C Soder. A comparison of the STORZ video laryngoscope and standard direct laryngoscopy for intubation in the Pediatric airway-a randomized clinical trial. Paediatr Anaesth 2009. [Google Scholar]
- F Javaherforooshzadeh, L Gharacheh. The Comparison of Direct Laryngoscopy and Video Laryngoscopy in Pediatric Airways Management for Congenital Heart Surgery: A Randomized Clinical Trial. Anesth Pain Med 2020. [Google Scholar]
- C Karsli, J Armstrong, J John. A comparison between the GlideScope® Video Laryngoscope and direct laryngoscope in paediatric patients with difficult airways-a pilot study. Anaesthesia 2010. [Google Scholar]
- ES Abid, J Mcnamara, P Hall, KA Miller, M Monuteaux, ME Kleinman. The Impact of Videolaryngoscopy on Endotracheal Intubation Success by a Pediatric/Neonatal Critical Care Transport Team. Prehosp Emerg Care 2021. [Google Scholar]
- MA Eisenberg, I Green-Hopkins, H Werner, J Nagler. Comparison between direct and video-assisted laryngoscopy for intubations in a pediatric emergency department. Acad Emerg Med 2016. [Google Scholar]
- JE Rabiner, M Auerbach, JR Avner, D Daswani, H Khine. Comparison of GlideScope videolaryngoscopy to direct laryngoscopy for intubation of a pediatric simulator by novice physicians. Emerg Med Int 2013. [Google Scholar] [Crossref]
- I Green-Hopkins, H Werner, MC Monuteaux, J Nagler. Using Video-recorded Laryngoscopy to Evaluate Laryngoscopic Blade Approach and Adverse Events in Children. Acad Emerg Med 2015. [Google Scholar]
- BT Kerrey, AS Rinderknecht, GL Geis, LE Nigrovic, MR Mittiga. Rapid sequence intubation for pediatric emergency patients: higher frequency of failed attempts and adverse effects found by video review. Ann Emerg Med 2012. [Google Scholar]
- M White, N Weale, J Nolan, S Sale, G Bayley. Comparison of the Cobalt Glidescope video laryngoscope with conventional laryngoscopy in simulated normal and difficult infant airways. Paediatr Anaesth 2009. [Google Scholar]
- T Lim, Y Lim, EHC Liu. Evaluation of ease of intubation with the GlideScope® or Macintosh laryngoscope by anaesthetists in simulated easy and difficult laryngoscopy. Anaesthesia 2005. [Google Scholar]
- TF Platts-Mills, D Campagne, B Chinnock, B Snowden, LT Glickman, GW Hendey. A comparison of GlideScope video laryngoscopy versus direct laryngoscopy intubation in the emergency department. Acad Emerg Med 2009. [Google Scholar]
